|
|
|
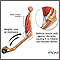
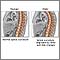
Osteoporosis |
| Definition: |
| Osteoporosis is a condition characterized by the progressive loss of bone density and thinning of bone tissue. |
| Alternative Names: |
| Thin bones
|
| Causes, incidence, and risk factors: |
|
Osteoporosis is the most common type of metabolic bone disease. There are currently an estimated 10 million Americans suffering from osteoporosis as well as another 18 million who have low bone mass, or osteopenia. Osteoporosis occurs when the body fails to form enough new bone, or when too much old bone is reabsorbed by the body, or both. Calcium and phosphate are two minerals that are essential for normal bone formation. Throughout youth, the body uses these minerals to produce bones. If calcium intake is not sufficient, or if the body does not absorb enough calcium from the diet, bone production and bone tissues may suffer. As people age, calcium and phosphate may be reabsorbed back into the body from the bones, which makes the bone tissue weaker. Both situations can result in brittle, fragile bones that are subject to fractures, even in the absence of trauma. Usually, the loss occurs gradually over years. Many times, a person will sustain a fracture before becoming aware that the disease is present. By the time this occurs, the disease is in its advanced stages and damage is profound. While there are a number of causes of osteoporosis, hormone deficiencies (estrogen in women and testosterone in men) are the leading cause. Women, especially over the age of 50, are the most frequent sufferers of the disease. This is due to the loss of ovarian function and subsequent reduction in estrogen production that occurs at the time of menopause. Other causes include corticosteroid excess from Cushing's syndrome, hyperthyroidism, hyperparathyroidism, immobilization, and bone malignancies. Researchers estimate that 13% to 18% of American women over the age of 50 have osteoporosis. In addition, 30% of them have osteopenia, which is abnormally low bone density that may eventually deteriorate into osteoporosis, if not treated. From these figures, researchers estimate that 50% of women over the age of 50 will suffer a fracture of the hip, wrist, or vertebra. Fewer men over the age of 50 have osteoporosis, with researchers estimating that 3-6% suffer from this disorder. In 1995, direct medical expenditures relating to osteoporotic fractures totaled $13.8 billion. Risk factors, in addition to menopause and advanced age, include genetic and ethnic background. Women who are white, especially those with a family history of osteoporosis, have a greater risk of developing osteoporosis. In fact, it is estimated that one out of two white women will experience a fracture relating to osteoporosis at some point in her life. Smoking, eating disorders, low body weight, low amount of calcium in the diet, heavy alcohol consumption, early menopause, absence of menstrual periods (amenorrhea), and use of certain medications, such as steroids and anticonvulsants, are also risk factors. |
| Symptoms: |
|
There are no symptoms associated with the early disease. As such, osteoporosis is a silent risk factor for fracture. Symptoms occurring late in the disease:
|
| Signs and tests: |
|
| Treatment: |
|
Treatments for osteoporosis focus on slowing down or stopping bone loss, preventing bone fractures by minimizing the risk of falls, and controlling pain associated with the disease. MEDICATIONS: BIPHOSPHONATES While side effects are generally mild, potential side effects include stomach upset and irritation of the esophagus. Because biphosphonates are difficult to absorb, these medicines should be taken on an empty stomach. The patient should not lie down or consume food or beverages (other than water) for at least 30 minutes after taking the medicine. The physician may also recommend taking calcium and Vitamin D supplements. Actonel is approved for use in men with osteoporosis. Both Actonel and Fosamax prevent and treat osteoporosis in men and women taking daily steroids for chronic conditions like asthma and arthritis. RALOXIFENE The most serious side effect of raloxifene is a very small risk of blood clots in the leg veins (deep venous thrombosis) or in the lungs (pulmonary embolus). ESTROGEN REPLACEMENT THERAPYEstrogen can slow or stop bone loss and, if estrogen treatment begins at menopause, it can reduce the risk of hip fractures up to 50%. Therapy is most effective if started at menopause, as most bone loss occurs 3-6 years after the onset of menopause. Many post-menopausal women choose estrogen replacement therapy (ERT) because of its proven usefulness in slowing the progress of or preventing osteoporosis. In some cases, ERT alleviates some of the irritating symptoms of menopause. This method of therapy is fairly inexpensive compared to the newer medications for osteoporosis discussed below. If estrogen replacement therapy is discontinued, bone loss will resume. Maximal protection from osteoporosis may indeed require lifelong dosing. Studies show that women who take estrogen for at least seven years between the onset of menopause and the age of 75 have a 50% reduction in risk of fractures. However after age 75, the risk is about the same as for those who did not take estrogen at all. In the 75 years and older group, bone mass only differs by about 2% between women who have taken estrogen for 10 years, and those who have never taken it. Some women hesitate to use estrogen supplements because of the numerous potential risks that have been associated with long-term use. Before beginning ERT, the benefits and consequences of the treatment should be weighed and discussed thoroughly with a health care provider. Women who have had a hysterectomy may take estrogen alone. Women with an intact uterus must take a combination of estrogen and progesterone. The decision to take estrogen for preservation of bone density is complicated by its effects on other diseases, including a relatively small increase in the risk of breast cancer. ERT has classically been thought to reduce the risk of coronary artery disease in post-menopausal women. Recent studies have brought controversy to this issue by providing evidence that women may have a higher incidence of coronary events during the first year on ERT. CALCITONIN While calcitonin slows bone loss and reduces the risk of fractures, it appears to be less effective than ERT or biphosphonates. As with some of the other newer medications, it is significantly more expensive than ERT. LIFESTYLE CHANGES: Regular exercise can reduce the likelihood of bone fractures associated with osteoporosis. Studies show that exercises requiring muscles to pull on bones cause the bones to retain and, perhaps, even gain density. Researchers found that women who walk a mile a day have four to seven more years of bone in reserve than women who don’t. Some of the recommended exercises include:
IMPORTANT: Any exercise that presents a risk of falling should be avoided. Fall prevention is an essential component of any comprehensive osteoporosis treatment program. Measures such as making sure the patient’s vision is good and appropriately corrected, avoiding sedating medications, and removing household hazards can significantly reduce the risk of fracture. Other ways to prevent falling include wearing good-fitting shoes, avoiding walking alone on icy days, and using bars in the bathtub, when needed. A diet that includes an adequate amount of calcium, Vitamin D, and protein should be maintained. While this will not completely stop bone loss, it will guarantee that a supply of the materials the body uses for bone formation and maintenance is available. Supplemental calcium should be taken as needed to achieve recommended daily calcium dietary intake. Current recommendations are for nonpregnant, menstruating women to consume 1000mg/day, pregnant women need 1200mg/day, and postmenopausal or nursing mothers should consume 1500 mg/day. High-calcium foods include low-fat milk, yogurt, ice cream and cheese, tofu, salmon and sardines (with the bones), and leafy green vegetables, such as spinach and collard greens. Vitamin D aids in calcium absorption and 400-800 IU per day should be taken by all individuals with increased risk of calcium deficiency and osteoporosis. MONITORING: Women taking estrogen should have routine mammograms, pelvic exams, and Pap smears. Patient response to treatment can be monitored with serial bone mineral density measurements every 1-2 years, though such monitoring is controversial, expensive, and not universally performed. In the future, use of less elaborate measurements of bone turnover, such as the N-telopeptide (Osteomark) urine test (discussed above) may become a standard means for following osteoporosis, though experience is presently limited. |
| Expectations (prognosis): |
|
Progression of the disease can sometimes be slowed or stopped with treatment. Some people become severely disabled, as a result of weakened bones. Hip fractures, which are frequently sustained by people with osteoporosis, leave about 50% of victims unable to walk independently. This is one of the major reasons people are admitted to nursing homes. Although osteoporosis is debilitating, it does not affect life expectancy. |
| Complications: |
|
| Calling your health care provider: |
|
Call your health care provider if you have symptoms of osteoporosis, or if you are interested in testing available for diagnosis or early detection. |
| Prevention: |
|
Throughout life, dietary intake of calcium is essential for bone formation and maintenance of healthy bone. Dietary Vitamin D, which aids in the absorption of calcium, is also essential. Maintaining a healthy diet as recommended by the FDA, which includes a sufficient amount of calcium, phosphorous, and Vitamin D, is very important. Avoiding smoking and excess alcohol consumption can help prevent osteoporosis. Regular exercise can reduce the likelihood of bone fractures. Studies show that exercises requiring muscles to pull on bones cause the bones to retain, and maybe even gain density. Post-menopausal women, especially those with reduced bone density, may consider intervention with estrogen replacement therapy. This may prevent bone loss or fracture in some people. There are a number of side effects associated with estrogen replacement therapy, and the option should be discussed thoroughly with your health care provider. A number of new medications for the prevention of osteoporosis, including raloxifene and alendronate, are currently available and FDA approved. |
Reviewed By: A.D.A.M. editorial (4/2/2002). Previous review: Sarah Pressman Lovinger, M.D., internist at Boston Medical Center, Boston, MA. Review provided by VeriMed Healthcare Network (1/18/2002).
 |
A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is the first of its kind, requiring compliance with 53 standards of quality and accountability, verified by independent audit. A.D.A.M. is among the first to achieve this important distinction for online health information and services. A.D.A.M. is also a founding member of Hi-Ethics (www.hiethics.com) and subscribes to the principles of the Health on the Net Foundation (www.hon.ch). |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 2003 A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.