|
|
|
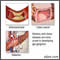
Gas gangrene |
| Definition: |
| A severe form of gangrene (tissue death) usually caused by Clostridium perfringens (see also necrotizing subcutaneous infection). It can also be from Group A Streptococcus. Staphlococcus aureus and Vibrio vulnificus can also cause similar infections.
|
| Alternative Names: |
| Tissue infection - Clostridial; Gangrene - gas; Myonecrosis; Clostridial infection of tissues |
| Causes, incidence, and risk factors: |
| Gas gangrene occurs as a result of infection by Clostridium bacteria that, under anaerobic (low oxygen) conditions, produce toxins that cause the tissue death and associated symptoms. Gas gangrene is rare, with only 1,000 to 3,000 cases occurring in the United States annually. Gas gangrene generally occurs at the site of trauma or a recent surgical wound. About a third of cases occur spontaneously. Patients who develop this disease spontaneously often have underlying vascular disease (atherosclerosis or hardening of the arteries), diabetes, or colon cancer. The onset of gas gangrene is sudden and dramatic. Inflammation begins at the site of infection as a pale to brownish-red and extremely painful tissue swelling. Gas may be felt in the tissue as a crackly sensation when the swollen area is pressed with the fingers. The margins of the infected area expand so rapidly that changes are visible over a few minutes. The involved tissue is completely destroyed. Clostridium bacteria produce many different toxins, 4 of which (alpha, beta, epsilon, iota) can cause potentially fatal syndromes. In addition, they cause tissue death (necrosis), destruction of blood (hemolysis), local decrease in circulation (vasoconstriction), and leaking on the blood vessels (increased vascular permeability). These toxins are responsible for both the local tissue destruction and the systemic symptoms (the other symptoms that occur throughout the body). Systemic symptoms develop early in the infection. These consist of sweating, fever, and anxiety. If untreated, the individual develops a shock-like syndrome with decreased blood pressure (hypotension), renal failure, coma, and finally death. |
| Symptoms: |
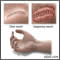
Note: Symptoms usually begin suddenly and rapidly worsen. |
| Signs and tests: |
|
Shock may be present, as evidenced by general pallor, cold extremities, low blood pressure, and rapid heart rate. Air in the tissues (crepitus) may be felt. Infection involving the entire body (systemic toxicity or sepsis) may develop. Yellow skin color associated with the excessive breakdown of blood cells (jaundice) is possible.
|
| Treatment: |
|
Prompt surgical removal of dead, damaged, and infected tissue (debridement) is necessary. Amputation of an arm or leg may be indicated to control the spread of infection. Antibiotics, preferably penicillin-type, should be given. Initially, this is given intravenously (through a vein). Analgesics may be required to control pain. Hyperbaric oxygen has been tried with varying degrees of success. |
| Expectations (prognosis): |
|
Gas gangrene is progressive and often lethal. Immediate medical attention is required. |
| Complications: |
| Calling your health care provider: |
|
Call your heath care provider if signs of infection occur at any time around a skin wound -- including pain, swelling, redness, drainage of pus or blood, fever, or similar symptoms. Go to the emergency room or call the local emergency number (such as 911), if symptoms indicate gas gangrene. This is an emergency condition requiring immediate medical attention! |
| Prevention: |
|
Clean any skin injury thoroughly. Watch for signs of infection (such as redness, pain, drainage, or swelling around a wound), and consult your health care provider promptly if these occur. |
Reviewed By: Camille Kotton, M.D., Infectious Diseases Division, Massachusetts General Hospital and Brigham and Women's Hospital, Boston, MA. Review provided by VeriMed Healthcare Network.
 |
A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is the first of its kind, requiring compliance with 53 standards of quality and accountability, verified by independent audit. A.D.A.M. is among the first to achieve this important distinction for online health information and services. A.D.A.M. is also a founding member of Hi-Ethics (www.hiethics.com) and subscribes to the principles of the Health on the Net Foundation (www.hon.ch). |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 2003 A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.