|
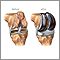
Knee joint replacement |
| Definition: |
| Surgery to replace a painful damaged or diseased knee joint with an artificial joint (prosthesis). |
| Alternative Names: |
| Total knee replacement; Knee arthroplasty |
| Description: |
|
The operation is performed under general anesthesia. The orthopedic surgeon makes an incision over the affected knee. The patella (knee cap) is moved out of the way, and the ends of the femur and tibia are cut to eliminate any rough parts and to permit a better adhesion of the prosthesis. The two parts of the prosthesis are implanted into the thigh bone (femur) and the tibia bone, using a special bone cement. Usually, metal is used on the end of the femur, and plastic is used on the tibia, for the new knee surface. However, newer surfaces including metal on both sides or ceramic on both sides are now being used. The patella is also resurfaced with plastic in some cases. Your leg will be placed in a continuous passive motion (CPM) device. This is a mechanical device that flexes (bends) and extends (straightens) the knee to keep the knee from getting stiff. Gradually, the rate and amount of flexion will be increased as tolerated. The leg should always be in this device when in bed. The CPM device helps speed recovery, decreases post-operative pain, bleeding and infection. The pain should gradually decrease, and by the third day after surgery, oral analgesic medications may be sufficient to control your pain. Try to schedule your pain medications about one half hour before walking or position changes. Prophylactic (preventive) antibiotics may be given to reduce the risk of developing an infection, necessitating removal of the artificial joint. Additionally, you will be encouraged to start moving and walking early after surgery. You will be assisted out of bed to a chair on the first day after surgery. When in bed, bend and straighten your ankles frequently to prevent development of blood clots. |
| Indications: |
Knee joint replacement may be recommended for:
|
| Risks: |
|
| Expectations after surgery: |
|
Results with a total knee replacement have been excellent. The operation relieves pain in over 90% of patients, and most need no assistance walking after recovery. Most prostheses last 10 to 15 years, some as long as 20 years, before loosening and requiring revision surgery. |
| Convalescence: |
|
The hospital stay generally lasts 4 or 5 days, but the total recovery period varies from 2-3 months to a year. Walking and range of motion exercises will be started immediately after surgery. Some surgeons recommend the use of a machine that will bend the knee for the patient in bed. Some patients require a short stay in a rehabilitation hospital to become safely independent in their activities of daily living. The use crutches or a walker for a few weeks or even months after surgery may be necessary. The physical therapy initiated in the hospital will continue after discharge until strength and motion return. Skiing and contact sports are generally to be avoided, but activities like swimming, tennis and golf are usually possible after full recovery from surgery. |
Reviewed By: Benjamin D. Roye, M.D., M.P.H., Department of Orthopaedics, New York-Presbyterian Hospital, New York, NY. Review provided by VeriMed Healthcare Network.
 |
A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is the first of its kind, requiring compliance with 53 standards of quality and accountability, verified by independent audit. A.D.A.M. is among the first to achieve this important distinction for online health information and services. A.D.A.M. is also a founding member of Hi-Ethics (www.hiethics.com) and subscribes to the principles of the Health on the Net Foundation (www.hon.ch). |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 2003 A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.