|
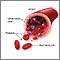
Bone marrow is found in a soft fatty tissue inside bones. This is where blood cells (red blood cells, platelets, and white blood cells) are produced and developed. If a patient develops a disease of the blood cells, especially cancers such as leukemia, he or she may require high doses of chemotherapy to destroy the cancer. However, this also destroys normal blood cells. Alternatively, hereditary or acquired disorders may cause abnormal blood cell production. In these cases, transplantation of healthy bone marrow may save a patient's life. Transplanted bone marrow will restore production of white blood cells, red blood cells, and platelets.
Bone marrow transplant patients are usually treated in specialized centers and the patient stays in a special nursing unit (bone marrow transplant unit: BMT) to limit exposure to infections.
Donated bone marrow must match the patient's tissue type. It can be taken from the patient, a living relative (usually a brother or a sister: allogeneic), or from an unrelated donor (found through the national marrow donor program which lists more than 700,000 potential donors). Donors are matched through special blood tests called HLA tissue typing (see HLA antigens).
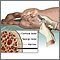
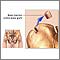
Bone marrow is taken from the donor in the operating room while the patient is unconscious and pain-free (under general anesthesia). Some of the donor's bone marrow is removed from the top of the hip bone (iliac crest). The bone marrow is filtered, treated, and transplanted immediately or frozen and stored for later use. Then, transplant material is transfused into the patient through a vein (IV line) and is naturally transported back into the bone cavities where it grows to replace the old bone marrow. Alternatively, blood cell precursors, called stem cells, can be induced to move from the bone marrow to the blood stream using special medications (mobilization). These stem cells can then be taken from the bloodstream through a procedure called leukapheresis.
The bone marrow recipient (the patient) is prepared for transplantation by administering high doses of chemotherapy and/or radiation (conditioning). This serves two purposes. First, it destroys the patient's abnormal blood cells or cancer. Second, it inhibits the patient's immune response against the donor bone marrow (graft rejection). Following conditioning, the patient is ready for bone marrow infusion. After infusion, it takes 10 to 20 days for the bone marrow to establish itself (engraft). During this time, the patient requires support with blood cell transfusions.
|