|
|
|
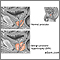
Prostate cancer |
| Definition: |
| Prostate cancer involves a malignant tumor growth within the prostate gland.
|
| Alternative Names: |
| Cancer - prostate |
| Causes, incidence, and risk factors: |
|
The cause of prostate cancer is unknown, although some studies have shown a relationship between high dietary fat intake and increased testosterone levels. When testosterone levels are lowered either by surgical removal of the testicles (castration, orchiectomy) or by medication, prostate cancer can regress. There is no known association with benign prostatic hyperplasia (BPH). Men at higher risk include black men older than 60, farmers, tire workers, painters, and men exposed to cadmium. The lowest incidence occurs in Japanese men and vegetarians.
This system also contains several substages. |
| Symptoms: |
|
With the advent of PSA testing, most prostate cancers are now found before they cause symptoms. Additionally, while most of the symptoms listed below can be associated with prostate cancer, they are more likely to be associated with non-cancerous conditions.
Additional symptoms that may be associated with this disease: |
| Signs and tests: |
|
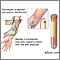
A rectal exam often reveals the hard, irregular surface of an enlarged prostate. Testing considerations:
A newer test called AMACR is more sensitive for determining the presence of prostate cancer than the PSA test and may become more widely used to diagnose disease. |
| Treatment: |
|
The appropriate treatment of prostate cancer is often controversial. Treatment options vary based on the stage of the tumor. In the early stages, surgical removal of the prostate (prostatectomy) and radiation therapy may be used to eradicate the tumor. Metastatic cancer of the prostate may be treated by hormonal manipulation (reducing the levels of testosterone by drugs or removal of the testes) or chemotherapy. SURGERY:
RADIATION THERAPY:
MEDICATIONS:
Synthetic drugs like Lupron or Zoladex that mimic the function of LHRH (luteinizing hormone releasing hormone) are being used increasingly to treat advanced prostate cancer. These medications suppress testostorone production. The procedure is often called "chemical castration" because it has the same result as surgical removal of the testes, although it is reversible, unlike surgery. The drugs must be given by injection, usually every three months. Possible side effects include nausea and vomiting, hot flashes, anemia, lethargy, osteoporosis, reduced sexual desire, and erectile dysfunction (impotence).
Surgery, radiation therapy, and hormonal manipulation all have the potential to disrupt sexual desire or performance on either a temporary or permanent basis. Discuss your concerns with your health care provider. Additionally, several options are available for managing sexual problems related to prostate cancer treatment. MONITORING: You will be closely monitored for progression of the disease regardless of the type of treatment you receive. Monitoring will include:
|
| Support Groups: |
| The stress of illness can often be helped by joining a support group where members share common experiences and problems. See support group - prostate cancer. |
| Expectations (prognosis): |
| The outcome varies greatly, primarily because the disease is found in older men who may have a variety of other complicating diseases or conditions (such as cardiac or respiratory disease and disabilities that immobilize or greatly decrease activities). |
| Complications: |
|
Impotence is a potential complication after prostatectomy or radiation therapy. Recent improvements in surgical procedures have made this complication occur less often. Urinary incontinence is another possible complication. Medications can have side effects, including hot flashes and loss of sexual desire. |
| Calling your health care provider: |
|
Call for an appointment if you are a man older than 50 and have:
You should discuss the advantages and disadvantages to PSA screening with your physician. |
| Prevention: |
|
No preventive measures are known. Adopting a vegetarian, low-fat diet or one that mimics the traditional Japanese diet may lower risk. Early identification (as opposed to prevention) is now possible by yearly screening of men over 40 or 50 years old through digital rectal examination (DRE) and PSA (prostate specific antigen) blood test. There is a debate however as to whether PSA testing should be done in all men. There are several potential downsides to PSA testing. The first is that elevated PSAs do not always mean a patient has prostate cancer. The second is that physicians may be detecting and treating some very early stage prostate cancers that would never have caused the patient any harm. The decision about whether to pursue a PSA should be based on a discussion between patient and physician. Each September is Prostate Cancer Awareness Month. Several urology centers across the country hold screening clinics that provide free rectal exams and PSA blood testing. Contact a hospital or medical center in your area for information on their program for Prostate Cancer Awareness. Additional information may be obtained by contacting your local chapter of the http://www.cancer.org/American Cancer Society. |
Reviewed By: A.D.A.M. editorial. Previous review: William Matsui, M.D., Department of Oncology, Johns Hopkins School of Medicine, Baltimore, MD. Review provided by VeriMed Healthcare Network. (5/16/2002)
 |
A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is the first of its kind, requiring compliance with 53 standards of quality and accountability, verified by independent audit. A.D.A.M. is among the first to achieve this important distinction for online health information and services. A.D.A.M. is also a founding member of Hi-Ethics (www.hiethics.com) and subscribes to the principles of the Health on the Net Foundation (www.hon.ch). |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 2003 A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.