|
|
|
Stroke |
| Definition: |
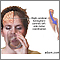
| A stroke is an interruption of the blood supply to any part of the brain, resulting in damaged brain tissue.
|
| Alternative Names: |
| Cerebrovascular disease; CVA; Cerebral infarction
|
| Causes, incidence, and risk factors: |
|
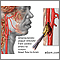
Stroke accounts for 1 out of every 15 deaths in the United States. It is the 3rd leading cause of death in most developed countries, and the leading cause of disability in adults. The risk doubles with each decade after age 35. Stroke occurs in men more often than women. If the flow of blood in an artery supplying the brain is interrrupted for longer than a few seconds, brain cells can die, causing permanent damage. The interruption can be caused by either bleeding or blood clots in the brain. A very common cause of stroke is atherosclerosis. (See stroke secondary to atherosclerosis.) Fatty deposits and blood platelets collect on the wall of the arteries, forming plaques. Over time, the plaques slowly begin to block the flow of blood. The plaque itself may block the artery enough to cause a stroke. In some cases, the plaque causes the blood to flow abnormally, which leads to a blood clot. A clot can stay at the site of narrowing and prevent blood flow to all of the smaller arteries it supplies. (This type of clot, which doesn't travel, is called a thrombus.) In other cases, the clot can travel and wedge into a smaller vessel. (A clot that travels is called an embolism.) Arrhythmias of the heart, such as atrial fibrillation, can be associated with this type of stroke and may contribute to clot formation. Other causes of embolic stroke include endocarditis (an infection of the heart valves), or use of a mechanical heart valve. A clot can form on the valve and break off and travel to the brain. A second major cause of stroke is bleeding in the brain (hemorrhagic stroke). This can occur when small blood vessels in the brain become weak and burst. Some people have defects in the blood vessels of the brain that makes this more likely. The flow of blood after the break damages brain cells. This kind of stroke can also occur if a clot caused by atherosclerosis or other conditions blocks a vessel, which then breaks and damages surrounding tissue. See also:
The risk of stroke is increased by smoking, hypertension, diabetes, hyperlipidemia, and heart disease. Medications that promote clot formation (e.g., birth control pills) may increase the risk, especially if a woman also smokes and is older than 35. Women have a higher risk of stroke during pregnancy and the weeks immediately after pregnancy. Other illnesses such as vasculitis, lupus or high blood viscosity may contribute to stroke. |
| Symptoms: |
|
The symptoms of stroke depend on how large an area of brain is affected and what part of the brain is injured. In some cases, persons may not be aware that they have had a stroke. The symptoms of stroke are most commonly a SUDDEN development of the following:
|
| Signs and tests: |
| In diagnosing a stroke, knowing how the symptoms developed is important. The symptoms may be severe at the beginning of the stroke, or symptoms may progress or fluctuate for the first day or two (stroke in evolution). Once there is no further deterioration, the stroke is considered a complete stroke. The exam will look for specific neurologic, motor, and sensory deficits, because these often correspond closely to the location of the injury to the brain. An examination may show changes in vision or visual fields, abnormal reflexes, abnormal eye movements, muscle weakness, decreased sensation, and other changes. A "bruit" (an abnormal sound heard with the stethoscope) may be heard over the carotid arteries of the neck. There may be signs of atrial fibrillation. Tests may determine the location and cause of the stroke and rule out other disorders that can cause the symptoms:
|
| Treatment: |
|
A stroke is a medical emergency. Physicians have begun to call it a "brain attack" to stress that getting treatment immediately can save lives and reduce disability due to stroke. Treatment varies, depending on the severity of symptoms. For virtually all strokes, hospitalization is required, possibly including intensive care and life support. IMMEDIATE TREATMENT In other circumstances, blood thinners such as heparin and coumadin are used to maintain circulation and to prevent recurrent strokes. Aspirin and other anti-platelet agents may be used to prevent strokes as well. Other medications may be needed to control associated symptoms. Analgesics may be needed to control severe headache. Anti-hypertensive medication may be needed to control high blood pressure. LONG-TERM TREATMENT The goal of treatment is to prevent the spread of the stroke and to maximize the patient's ability to function. The recovery time and need for long-term treatment vary. The individual's safety must be considered. Some people with stroke appear to have no awareness of their surroundings on the affected side. Others show a marked indifference or lack of judgment, which increases the need for safety precautions. For these people, friends and family members should repeatedly reinforce important cues, like name, age, date, time, and where they live to help reduce disorientation. Communication may require pictures, demonstration, verbal cues or other strategies, depending on the type and extent of language deficit. In-home care, boarding homes, adult day care, or convalescent homes may be required to provide a safe environment, control aggressive or agitated behavior, and meet physiological needs. Behavior modification may be helpful for some people in controlling unacceptable or dangerous behaviors. Family counseling may help in coping with the changes required for home care. Visiting nurses or aides, volunteer services, homemakers, adult protective services, and other community resources may be helpful. Legal advice may be appropriate. Advance directives, power of attorney, and other legal actions may make it easier to make ethical decisions regarding the care of the person with organic brain syndromes such as stroke. Carotid endarterectomy, removal of plaque from the carotid arteries, may help prevent new strokes from occurring in some people. |
| Support Groups: |
|
Additional support and resources are available from the http://www.strokeassociation.org/American Stroke Association. The toll-free phone line for stroke survivors and caregivers is 1-888-4STROKE |
| Expectations (prognosis): |
| Stroke is the third leading cause of death in developed countries. The long-term outlook depends on the extent of damage, associated medical problems, and the likelihood of recurring strokes. Of those who survive a stroke, many have long-term disabilities, but some may recover most or all function. |
| Complications: |
|
| Calling your health care provider: |
| Call the local emergency number (such as 911) to be taken to the emergency room if you have symptoms of a stroke. Stroke requires immediate treatment. |
| Prevention: |
|
Stroke prevention involves controlling risk factors and treating medical problems that can cause blood clotting:
|
Reviewed By: Joseph V. Campellone, M.D., Division of Neurology, Cooper Hospital/University Medical Center, Camden, NJ. Review provided by VeriMed Healthcare Network.
 |
A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is the first of its kind, requiring compliance with 53 standards of quality and accountability, verified by independent audit. A.D.A.M. is among the first to achieve this important distinction for online health information and services. A.D.A.M. is also a founding member of Hi-Ethics (www.hiethics.com) and subscribes to the principles of the Health on the Net Foundation (www.hon.ch). |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 2003 A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.