|
|
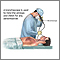
Bronchoscopy |
| Definition: |
| Bronchoscopy is a diagnostic procedure in which a tube with a tiny camera on the end is inserted through the nose or mouth into the lungs. The procedure provides a view of the airways of the lung and allows doctors to collect lung secretions and to biopsy for tissue specimens. |
| Alternative Names: |
| Fiberoptic bronchoscopy |
| How the test is performed: |
|
The pulmonologist (a lung specialist trained to perform a bronchoscopy) sprays a topical or local anesthetic in your mouth and throat. This will cause coughing at first, which will cease as the anesthetic begins to work. When the area feels "thick," it is sufficiently numb. Medications to relax you may be given through an IV, making you sleepy. Usually, a flexible bronchoscope is used. The flexible tube is less than 1/2-inch wide and about 2-feet long. As the bronchoscope is used to examine the airways of the lungs, your doctor can obtain samples of your lung secretions to send for laboratory analysis. Saline solution can be introduced to flush the area and collect cells that may be analyzed by a pathologist or microbiologist. This part of the procedure is called a "lavage" or a bronchial washing. Usually, small amounts (5-10 cc, or 1-2 teaspoons) of saline are used. In certain circumstances, a larger volume of saline may be used. In this procedure, called bronchoalveolar lavage, up to 300 cc of saline (20 tablespoons) are instilled into the airway after the bronchoscope has been advanced as far as possible and a small airway is completely blocked (temporarily) by the scope. Bronchoalveolar lavage is performed to obtain a sample of the cells, fluids, and other materials present in the very small airways and alveoli (air sacs). In addition, tiny brushes, needles, or forceps can be introduced through the bronchoscope to obtain tissue samples from your lungs. Occasionally, stenting and laser therapies can be performed through the bronchoscope. A rigid bronchoscope is less commonly used, and usually requires general anesthesia. |
| How to prepare for the test: |
|
This test may require an overnight stay in the hospital. A list of essentials is usually available from a doctor or clinic. Fasting is required for 6 to 12 hours before the test. Your doctor may want you to avoid any aspirin or ibuprofen-type medications before the procedure. You must sign an informed consent form. Arrange for transportation to and from the hospital. Many people want to rest the following day, so make arrangements for work, child care, or other obligations.
|
| How the test will feel: |
|
Local anesthesia is used to relax the throat muscles, so there is the feeling of fluid running down the back of the throat and the need to cough or gag until the anesthetic begins working. When the anesthetic wears off, the throat may be scratchy for several days. After the test, the cough reflex will return in 1 to 2 hours, then normal eating and drinking is allowed. |
| Why the test is performed: |
| This test is recommended if a chest X-ray or other diagnostic procedure suggests a lung disease that requires an inspection of the airways of the lung or a tissue sample for diagnosis. Bronchoscopy is also recommended if you have been coughing up blood (hemoptysis). |
| Normal Values: |
|
The trachea and bronchi have normal cells and secretions and no foreign bodies or obstructions. |
| What the risks are: |
|
The main risks from bronchoscopy are:
There is also a small risk of:
In the rare instances when general anesthesia is used, there is some risk for:
There is a small risk for: When a biopsy is taken, there is a risk of hemorrhage. Some bleeding is common. However, the technician or nurse will monitor the amount of bleeding. |
| Special considerations: |
|
Your gag reflex should return before drinking or eating anything after the bronchoscopy. To test if the gag reflex has returned, place a spoon on the back of your tongue for a few seconds with light pressure. If there is no gagging, wait 15 minutes and attempt it again. Make sure that no small or sharp objects are used to test this reflex. |
Reviewed By: David A. Kaufman, M.D., Pulmonary & Critical Care Medicine, University of Pennsylvania Medical Center, Philadelphia, PA. Review provided by VeriMed Healthcare Network.
 |
A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is the first of its kind, requiring compliance with 53 standards of quality and accountability, verified by independent audit. A.D.A.M. is among the first to achieve this important distinction for online health information and services. A.D.A.M. is also a founding member of Hi-Ethics (www.hiethics.com) and subscribes to the principles of the Health on the Net Foundation (www.hon.ch). |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 2003 A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.