|
|
|
Heart failure |
| Definition: |
|
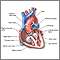
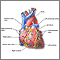
Heart failure, also called congestive heart failure, is a disorder in which the heart loses its ability to pump blood efficiently. The term "heart failure" should not be confused with cardiac arrest, a situation in which the heart actually stops beating. |
| Alternative Names: |
| CHF; Congestive heart failure |
| Causes, incidence, and risk factors: |
|
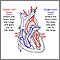
Heart failure is almost always a chronic, long-term condition, although it can sometimes develop suddenly. This condition may affect the right side, the left side, or both sides of the heart. As the heart's pumping action is lost, blood may back up into other areas of the body:
With heart failure, many organs don't receive enough oxygen and nutrients, which damages them and reduces their ability to function properly. Most areas of the body can be affected when both sides of the heart fail. The most common causes of heart failure are the chronic cardiovascular diseases hypertension (high blood pressure) and coronary artery disease. Other structural or functional causes of heart failure include the following:
Approximately 2 out of every 100 people between the ages of 27 and 74 have heart failure. Heart failure becomes more common with advancing age. |
| Symptoms: |
Infants may sweat during feeding (or other exertion). Symptoms may not be present in all patients with heart failure. In people with asymptomatic heart failure, symptoms may develop only after certain factors appear, including the following:
Other risk factors include obesity, excessive alcohol consumption, and a high-salt diet. |
| Signs and tests: |
| A physical examination may reveal either an irregular or a rapid heartbeat. There may be distended neck veins, enlarged liver, peripheral edema (swelling of the limbs), and signs of pleural effusion (fluid around the lungs).
Listening to the chest with a stethoscope (auscultation) may reveal lung crackles or abnormal heart sounds. Blood pressure may be normal, elevated or low.
This disease may also alter the following test results:
If excessive fluid has accumulated around the sac surroundig the heart (pericardium), you may need to have the fluid removed through a pericardiocentesis. |
| Treatment: |
|
Heart failure requires monitoring of the condition by the health care provider. The first step is usually to identify and treat any underlying disorders and precipitating factors. This may require a thorough diagnostic work-up, medications or certain medical procedures (catheter procedures or surgery). The goals of treatment in heart failure include reduction of the heart's workload, control of excess salt and water retention (swelling, decreased urinary output) and improvement of heart function. In advanced cases or when the heart failure occurs suddenly (acute heart failure), bed rest or reduced physical activity are recommended to minimize the heart's workload. Digoxin may also be given, especially if the heart rhythm is irregular due to atrial fibrillation. Medications used to reduce the heart's workload include angiotensin converting enzyme (ACE) inhibitors such as captopril and enalapril, and angiotensin receptor blockers such as losartan and candesartan. Other medications frequently used are vasodilators such as hydralazine and long-acting nitrates. Some patients, particularly those with a history of coronary artery disease, may benefit from low doses of beta-blockers. Weight loss may be recommended for overweight patients. Eliminate smoking and excessive alcohol consumption (which decrease the pumping efficiency of the heart). The heart's ability to pump blood can be directly increased by medications called inotropic agents. These include dobutamine and milrinone, which are given intravenously. Unstable patients receiving several medications usually need also hemodynamic monitoring with Swan-Ganz catheterization. Severe cases require more drastic measures. For example, excess fluid can be removed through dialysis, and circulatory assistance can be provided by implanted devices such as the intra-aortic balloon pump (IABP) and the left ventricular assist device (LVAD). These devices can be life-saving, but they are not permanent solutions. Patients who become dependent on circulatory support will need a heart transplant. |
| Expectations (prognosis): |
| Heart failure is a serious disorder that carries a reduced life expectancy. Many forms of heart failure can be controlled with medication and correction of underlying disorders. Heart failure is usually a chronic illness, and it may worsen with infection or other physical stressors. |
| Complications: |
|
| Calling your health care provider: |
|
Call your health care provider if you have symptoms of congestive heart failure. |
| Prevention: |
| Follow your health care provider's recommendations for treatment of conditions that may cause congestive heart failure. Follow dietary guidelines. Minimize or eliminate smoking and alcohol consumption. |
Reviewed By: Elena Sgarbossa, M.D., Department of Cardiology, Cleveland Clinic Florida, Weston, FL. Review provided by VeriMed Healthcare Network.
 |
A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is the first of its kind, requiring compliance with 53 standards of quality and accountability, verified by independent audit. A.D.A.M. is among the first to achieve this important distinction for online health information and services. A.D.A.M. is also a founding member of Hi-Ethics (www.hiethics.com) and subscribes to the principles of the Health on the Net Foundation (www.hon.ch). |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 2003 A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.