|
|
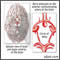
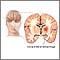
Intracerebral hemorrhage |
| Definition: |
| Intracerebral hemorrhage involves bleeding in the brain caused by the rupture of an intracranial (within the head) blood vessel. See also hemorrhagic stroke.
|
| Alternative Names: |
| Intracranial hemorrhage; Hemorrhage - intracerebral; Hypertensive hemorrhage
|
| Causes, incidence, and risk factors: |
|
Internal bleeding can occur in any part of the brain. Blood may accumulate in the brain tissues or in the space between the brain and the membranes covering the brain (subarachnoid space). The bleeding may be isolated to part of one cerebral hemisphere (lobar intracerebral hemorrhage) or it may occur in other brain structures, such as the thalamus, basal ganglia, pons, or cerebellum (deep intracerebral hemorrhage). Other factors that raise the risk of intracerebral hemorrhage include the following:
Premature infants (born earlier than 35 weeks gestation) will sometimes have bleeding into the ventricles (fluid-filled spaces) in the brain. This type of bleed is called intra-ventricular hemorrhage (IVH). This occurs in the first day or so of life and is usually not preventable. The outcome is variable, depending on the severity of bleed and ranges from no apparent damage to severe disability. Diagnosis is by ultrasound and usually done in an intensive care nursery. |
| Symptoms: |
|
| Signs and tests: |
| Neuromuscular examination may indicate increased intracranial pressure or focal neurologic deficits (decreases in brain function). The specific pattern of symptoms and function changes may indicate the location of the intracerebral hemorrhage. Eye examination may show optic nerve swelling caused by increased pressure in the brain, or there may be changes in eye movement. Abnormal reflexes may be present, or there may be an abnormal extent of normal reflexes. Tests to determine the amount and cause of bleeding may include the following:
|
| Treatment: |
| Intracerebral hemorrhage is a severe condition requiring prompt medical attention even if symptoms are episodic (occurring occasionally, then disappearing). It may develop quickly into a life-threatening situation. Treatment goals include lifesaving interventions, supportive measures and control of symptoms. Treatment varies, depending on the specific location, extent, and cause of the bleeding. Surgical removal of hematomas may be appropriate, especially if there is a hematoma in the cerebellum. Surgical repair of structures causing the bleed (repair of aneurysm, arteriovenous malformation) may be appropriate in some cases. Medicines used may include corticosteroids or diuretics to reduce swelling, anticonvulsants to control seizures, analgesics to control pain and others. Blood, blood products, intravenous fluids, or medications may be appropriate to counteract bleeding and loss of blood volume. |
| Expectations (prognosis): |
| The outcome varies highly. Death may occur rapidly despite prompt medical treatment. Recovery may occur completely or with a permanent loss of some brain functions. Medications, surgery or treatments for this condition can have severe side effects. |
| Complications: |
|
| Calling your health care provider: |
| Go to the emergency room or call the local emergency number (such as 911) if symptoms indicate intracerebral hemorrhage. This is a life-threatening condition. Emergency symptoms include: |
| Prevention: |
|
Treatment and control of causative and risk-related disorders may reduce the risk of developing intracerebral hemorrhage. High blood pressure should be treated. Do not stop taking medications unless advised to do so by your health care provider. Known vascular malformations such as an aneurysm can often be treated before they cause bleeding in the brain. |
Reviewed By: Elaine T. Kiriakopoulos, M.D., MSc, Department of Neurology, Beth Israel Deaconess Medical Center, Harvard University, Boston, MA. Review provided by VeriMed Healthcare Network.
 |
A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is the first of its kind, requiring compliance with 53 standards of quality and accountability, verified by independent audit. A.D.A.M. is among the first to achieve this important distinction for online health information and services. A.D.A.M. is also a founding member of Hi-Ethics (www.hiethics.com) and subscribes to the principles of the Health on the Net Foundation (www.hon.ch). |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 2003 A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.