|
|
|
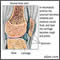
Rheumatoid arthritis |
| Definition: |
| A chronic inflammatory disease that primarily affects the joints and surrounding tissues, but can also affect other organ systems. |
| Alternative Names: |
| RA |
| Causes, incidence, and risk factors: |
|
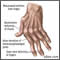
The cause of rheumatoid arthritis (RA) is unknown, however the condition involves an attack on the body by its own immune cells (auto-immune disease). Different cases may have different causes. Infectious, genetic, and hormonal factors may play a role. The disease can occur at any age, but the peak incidence of disease onset is between the ages of 25 and 55. The disease is more common in older people. Women are affected 2.5 times more often than men. Approximately 1-2% of the total population is affected. The course and the severity of the illness can vary considerably. The onset of the disease is usually gradual, with fatigue, morning stiffness (lasting more than one hour), diffuse muscular aches, loss of appetite, and weakness. Eventually, joint pain appears, with warmth, swelling, tenderness, and stiffness of the joint after inactivity. Joint involvement in RA usually affects both sides of the body equally -- the arthritis is therefore referred to as symmetrical. Wrists, fingers, knees, feet, and ankles are the most commonly affected joints. Severe disease is associated with larger joints that contain more synovium (joint lining). When the synovium becomes inflamed, it secretes more fluid and the joint becomes swollen. Later, the cartilage becomes rough and pitted. The underlying bone eventually becomes affected. Joint destruction begins 1-2 years after the appearance of the disease. Characteristic deformities result from cartilage destruction, bone erosions, and tendon inflammation and rupture. A life-threatening joint complication can occur when the cervical spine becomes unstable as a result of RA. Other features of the disease that do not involve the joints may occur. Rheumatoid nodules are painless, hard, round or oval masses that appear under the skin, usually on pressure points, such as the elbow or Achilles tendon. These are present in about 20% of cases and tend to reflect more severe disease. On occasion, they appear in the eye where they sometimes cause inflammation. If they occur in the lungs, inflammation of the lining of the lung (pleurisy) may occur, causing shortness of breath. Anemia may occur due to failure of the bone marrow to produce enough new red cells to make up for the lost ones. Iron supplements will not usually help this condition because iron utilization in the body becomes impaired. Other blood abnormalities can also be found, for example, platelet counts that are either too high or too low. Rheumatoid vasculitis (inflammation of the blood vessels) is a serious complication of RA and can be life-threatening. It can lead to skin ulcerations (and subsequent infections), bleeding stomach ulcers (which can lead to massive hemorrhage), and neuropathies (nerve problems causing pain, numbness or tingling). Vasculitis may also affect the brain, nerves, and heart causing strokes, sensory neuropathies (numbness and tingling), heart attacks, or heart failure. Heart complications of RA commonly affect the outer lining of the heart. When inflamed, the condition is referred to as pericarditis. Inflammation of heart muscle, called myocarditis, can also develop. Both of these conditions can lead to congestive heart failure characterized by shortness of breath and fluid accumulation in the lung. Lung involvement is frequent in RA. Fibrosis of the lung tissue leads to shortness of breath and has been reported to occur in 20% of patients with RA. Inflammation of the lining of the lung, called pleuritis, can also lead to fluid accumulation. Pulmonary nodules, similar to rheumatoid nodules, can also develop. Eye complications include inflammation of various parts of the eye. These must be screened for in RA patients. |
| Symptoms: |
|
| Signs and tests: |
|
| Treatment: |
| RA usually requires lifelong treatment, including various medications, physical therapy, education, and possibly surgery aimed at relieving the signs and symptoms of the disease.
MEDICATIONS: Anti-inflammatory agents used to treat RA traditionally included aspirin and non-steroidal anti-inflammatory drugs (NSAIDS), such as ibuprofen (Motrin, Advil), fenoprofen, indomethacin, naproxen (Naprosyn), and others. These are widely used medications that are effective in relieving pain and inflammation associated with RA. However, side effects associated with frequent use of many of these medications include life-threatening gastrointestinal bleeding. Similar drugs, called Cox-2 inhibitors, are now a mainstay of anti-inflammatory therapy because the risk of gastrointestinal bleeding is significantly reduced with these drugs. Currently, there are two available -- rofecoxib (Vioxx) and celecoxib (Celebrex). As mentioned, DMARDs alter the course of the disease. Included in this group are gold compounds, which can be injectible (Myochrysine and Solganal) or oral (auranofin/Ridaura). Methotrexate (Rheumatrex) is the most commonly used DMARD for rheumatoid arthritis with good proven effectiveness. Antimalarial medications, such as Hydroxychloroquine (Plaquenil), as well as Sulfasalazine (Azulfidine), are also beneficial, usually in conjunction with Methotrexate. The benefits from these medications may take weeks or months to be apparent. Because they are associated with toxic side effects, frequent monitoring of blood tests while on these medications is imperative. In the last few years, new and exciting medications have been introduced. A promising medication that is fast becoming a first-line agent for the aggressive treatment of RA is called etanercept (Enbrel). Enbrel acts by inhibiting an inflammatory protein, called tumor necrosis factor (TNF). Other new medications include infliximab (Remicade) that also blocks TNF and leflunomide (Arava), which blocks the growth of new cells. Anakinra is an even newer therapy that blocks the action of another inflammatory protein, interleukin-1. Anakinra and Etanercept are injectable medications, whereas Infliximab is given intravenously every 2 months. Drugs that suppress the immune system, like azathioprine (Imuran) and cyclophosphamide (Cytoxan), may be used in people who have failed other therapies. These medications, which are associated with toxic side effects, are reserved for severe cases of RA. Corticosteroids have been used to reduce inflammation in RA for greater than 40 years. However, because of potential long-term side effects, corticosteroid use is limited to short courses and low doses where possible. Side effects may include bruising, psychosis, thinning of the bones (osteoporosis), cataracts, weight gain, susceptibility to infections, diabetes, and high blood pressure. A number of medications can be administered in conjunction with steroids to minimize resultant osteoporosis. Consult a health care provider before long-term use of any medication, including over-the-counter medications. SURGERY: A later alternative is total joint replacement with a joint prosthesis. Surgeries can be expected to relieve joint pain, correct deformities, and modestly improve joint function. In extreme cases, total knee or hip replacement can mean the difference between being totally dependent on others and having an independent life at home. LIFESTYLE CHANGES: Range of motion exercises and individualized exercise programs prescribed by a physical therapist can delay the loss of joint function. OTHER THERAPY: Prosorba column is a device approved by the FDA in 1999 for treatment of moderate to severe RA in adult patients with long-standing disease (who have not responded to DMARD's). It works by removing inflammatory antibodies from the blood by a process called apheresis. The blood is removed through a small catheter and then passed through a column (the size of a coffee mug) that is coated with a substance called protein A. Protein A binds with the antibodies and removes them from the blood. The blood is then given back. The procedure takes 2-3 hours, and must be done once a week for 12 weeks. Studies have reported that one third to one half of the people who receive this treatment may slow down, or even stop the RA from worsening. Reported side effects include anemia, fatique, fever, low blood pressure, and nausea. Some people have developed an infection from the catheter. Often there is a flare-up of joint pain for several days after the treatment. Sometimes therapists will use special machines to apply deep heat or electrical stimulation to reduce pain and improve joint mobility. MONITORING: Depending on the medications being taken, regular blood or urine tests should be done to monitor both progress and negative side effects. |
| Support Groups: |
|
The stress of illness can often be helped by joining a support group in which members share common experiences and problems. See arthritis - support group. |
| Expectations (prognosis): |
|
Frequently, the disease can be controlled with a combination of treatments. Treatment may vary depending on the severity of the symptoms. Surgery may be needed, if medications fail. The course of the disease varies between individuals. People with rheumatoid factor and/or subcutaneous nodules seem to have a more severe course of disease. People who develop RA at younger ages also have a more rapidly progressive course. Remission is most likely to occur in the first year and the probability decreases as time progresses. By 10 to 15 years from diagnosis, about 20% of people will have had remission. Between 50 - 70% will remain capable of full-time employment. After 15 to 20 years, only 10% of patients are severely disabled, and unable to perform simple activities of daily living (washing, toileting, dressing, eating). However, the average life expectancy may be shortened by 3 to 7 years with this disease, and patients with severe forms of RA may die 10-15 years earlier than expected. As treatment for rheumatoid arthritis improves, the occurrence of severe disability and life threatening complications appears to be decreasing, so these figures may be overly pessimistic. |
| Complications: |
|
Rheumatoid arthritis is not solely a disease of joint destruction. It can involve almost all organ systems. The treatments for RA have also yielded serious side effects. Quality of life can be reduced, and mortality can increase. As mentioned previously, the complications of RA can include joint destruction, gastrointestinal bleeding, heart failure, pericarditis, pleuritis, lung disease, anemia, low or high platelets, eye disease, cervical (neck) spine instability, neuropathy, and vasculitis. Fortunately, improved therapies appear to be reducing the occurrence of these severe complications. |
| Calling your health care provider: |
|
Call your health care provider if you think you have symptoms of rheumatoid arthritis. |
| Prevention: |
|
Rheumatoid arthritis has no known prevention. However, it is often possible to prevent further damage of the joints with proper early treatment. |
Reviewed By: A.D.A.M. editorial. Previous review: Ajay Nirula M.D., Ph.D., Department of Rheumatology, University of California San Francisco, San Francisco, CA. Review provided by VeriMed Healthcare Network (1/31/2002).
 |
A.D.A.M., Inc. is accredited by URAC, also known as the American Accreditation HealthCare Commission (www.urac.org). URAC's accreditation program is the first of its kind, requiring compliance with 53 standards of quality and accountability, verified by independent audit. A.D.A.M. is among the first to achieve this important distinction for online health information and services. A.D.A.M. is also a founding member of Hi-Ethics (www.hiethics.com) and subscribes to the principles of the Health on the Net Foundation (www.hon.ch). |
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed physician should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. Copyright 2003 A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.